
Your Health Care

Health care plans, policies, and assistance are intended to protect you and your family from catastrophic medical expenses. We define each type of health care coverage below. It is important to be able to distinguish the differences among each type.
Employer-Provided Health Care Plans
For these plans, your employer, not an insurance company, foots the bill for all employees’ medical costs. In some types of employer-provided health care plans, the employer also bears the financial risk of insuring you and your family. These types of employer-provided plans are called “self insured plans.” Your employer pays a health care administrator, a company that specializes in administering health care plans, to process your medical claims.
To participate in an employer-provided health care plan, you pay a monthly amount through paycheck deductions. In addition to these deductions, you are also typically financially responsible for:
- A co-pay: a portion of the cost to visit a health care provider.
- Co-insurance: a portion of the cost of health care services. A typical co-insurance requirement is 80/20. This means that your health care plan would pay for 80 percent of your health care expenses; you would pay for the remaining 20 percent.
- An annual deductible: an amount you pay each year before your health care plan starts paying for your medical services.
Insurance Health Care Policies
These are purchased from private insurance companies, usually through your employer or directly through an insurance agent. The insurance company bears the risk of insuring you and your family. You pay for insurance policies with monthly premiums. If your insurance is purchased through your employer, your monthly premium is usually automatically deducted from your paycheck and your employer pays the insurance company for you. Some employers pay for all or a portion of your monthly premium. Whether you or your employer pays your monthly premium, you are typically financially responsible for co-pays, co-insurance, and an annual deductible.
Government Health Care Assistance
This is insurance coverage provided through government agencies, such as Medicaid. It is financed by federal and state governments, but administered by the states. This means each state’s health care assistance program may have a unique name. Contact your county’s Office of Public Assistance or Social Services to find out about your state’s health care assistance program. Also, each state varies in program eligibility requirements, what types of services are covered, and how those services are paid for.
Note! For simplicity, throughout this publication, we collectively refer to the three types of health care coverage explained above as “health care plan."
HealthCare.gov
HealthCare.gov is a comprehensive web site for all individuals who need help:
- Finding insurance options
- Comparing different types of health care
- Learning about ways to stay healthy
- Learning about new health reform legislation
HealthCare.gov has a section devoted to individuals with disabilities.
Visit www.HealthCare.gov for more information.
Family-to-Family Health Information Centers
Figuring out who to contact, what your health care benefits are, and how much they cost is a challenge. Funded by the Health Resources and Services Administration, Maternal Child Health Bureau, Family-to-Family Health Information Centers located in each state offer parents go-to resources for navigating and working effectively with various health care systems. Each state’s center offers parents resources based on what health care services the state provides. The mission of each family center is to help parents make informed health care choices for their children with special needs.
To find the Family-to-Family Health Information Center in your state, contact Family Voices, Inc:
Call 1-888.835-5669
Visit www.FamilyVoices.org and click “State FV”
Write
P.O. Box 37188
Albuquerque, NM 87176
Your Medical Coverage
Your medical expenses may place one of the biggest and most stressful demands on your financial well-being. Whether you receive health care benefits from an employer, an insurance company, or a government health care assistance program, you want to get the very most out of the coverage you have. To do that, it is essential you completely and clearly understand the provisions of your health care plan.
Your Summary of Benefits and Explanation of Benefits (EOB)
These are your most important medical documents. Keep them in one convenient place.
The Summary of Benefits describes in detail what medical conditions and services will be covered, for what amounts, and your financial responsibilities. The Explanation of Benefits (EOB) describes in detail your benefits for a particular service or health care provider’s visit.
Documentation on medical coverage is complex. By breaking it down into chunks of information—it won’t seem so overwhelming. Here are the essential pieces:
- Your benefits: what is covered, or not
- Your financial responsibilities for doctor’s visits, prescriptions, hospital care, any special treatments or therapies your family requires, and assistive technologies
- Your health care plan’s financial responsibilities
- How your claims are paid
- How to appeal a denied claim
Your doctor’s office will usually file medical claims for you (notify your health care plan administrator of the services you received). In some cases, you have to send in your own claims. After your health care plan administrator receives your claim, it will process it. That means your health care plan administrator, based on the service you received and the benefits of your plan, determines:
- The dollar amount of the service it will cover
- The percentage of that amount it will pay for
- The percentage of that amount you must pay for
How Deductibles Work
This is a very simple explanation of how deductibles work. Other health care plan conditions may affect how deductibles are applied.
Say your annual deductible amount is $500. That means you must pay for the first $500 worth of medical services you receive for any year. So you visit your doctor and it costs $1,000. Let’s also say that (1) you are responsible for a $25 co-pay for each doctor’s visit, and (2) your health care plan will pay for 100 percent of this visit.
When you receive your EOB, the calculation of how much you and your health care plan will each pay might look something like this:
Cost of Visit: $1,000
Less: $500 deductible (you pay this)
Subtotal: $50
Less Co-Pay: $25 (you pay this)
Your Benefit: $475 (your health care plan pays this)
After you’ve paid the bill for this visit, you’ve completely paid your deductible for the year. The next time you have this same type of visit, it will only cost you $25, the co-pay, because your health care plan pays 100 percent for that type of visit.
Every January or on your plan’s anniversary (the day your benefit plan went into effect), the deductible goes back to zero. That means you again pay the first $500 of medical service for that year. A deductible may be spread over a series of health care visits until you pay the full deductible amount.
Sample Information on an Explanation of Benefits Document
Say a doctor’s visit for a check-up costs $200. Your health care plan may only cover 80 percentage of that check-up amount, or $160. You would pay the difference of $40.
Of that $160, your health care plan may pay for half of it, or $80. You would pay for the difference, or $80.
Adding those two payments of $40 and $80 together, you would be financially responsible for $120 of that $200 doctor’s visit; your health care plan is responsible for $80.
Your health care plan administrator will summarize all this on an Explanation of Benefits (EOB) statement, indicating the total amount you owe. This statement is not a bill, merely an explanation of your coverage and who is financially responsible for what. Your EOB will also contain information on how to appeal a claim. You will want to appeal a claim, or ask your health care plan administrator to review your claim again, if you were denied coverage you believe you are entitled to..
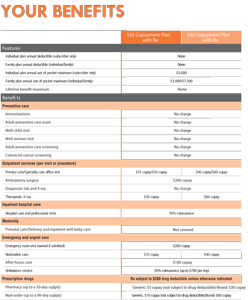
Types of Employer-Provided and Private Insurance Health Care Plans

Employers and private insurance companies offer a variety of benefit plans. We’ll explain five types of them below, stating for each its typical plan features. Nearly all plans are variations of these five types, though. Use this information as a quick reference. Your health care plan documentation will provide a more accurate description of your health care benefits.
Health Maintenance Organization (HMO)
This type of plan is the most restrictive in what doctors you can see and the type of health care offered. HMOs cover expenses related to an illness and offer preventive care services such as check-ups, well-baby care, and mammograms. Some government health care assistance programs require that plan beneficiaries use specific HMOs for their services. If you have an HMO, you must:
- Use doctors employed by the HMO. Ask an HMO representative about the plan’s policy for seeing doctors not employed by the HMO.
- Use hospitals affiliated with the HMO except for out-of-town emergencies.
- Make co-payments for each doctor’s visit, typically $10–$30.
It is also important to know what your plan’s policy is on seeing both in- and out-of-network specialists. Speak with your primary care physician or an HMO representative about this before seeking a specialist. Your doctor’s office usually submits claims to the HMO for you. The HMO in turn sends you an Explanation of Benefits (EOB).
Preferred Provider Organization (PPO)
This type of plan offers a wider access to doctors and may offer some coverage to alternative types of health care, such as acupuncture. PPOs cover expenses related to an illness and typically offer some preventive care services. Under this plan you:
- Use doctors who are members of the PPO’s network.
- Make co-payments for each doctor’s visit, typically $25–$45.
- May need permission from your primary care physician to see a specialist who is a member of the network.
- Have the option to see out-of-network providers (doctor’s and specialists who are not members of the PPO). Permission to see them is usually not required, but you will pay an additional cost to see out-of-network providers.
Your doctor’s office usually submits your claims to the PPO for you. The PPO in turn sends you an EOB.
Point-of-Service Plan (POS)
This type of plan is the most flexible of all. Its features are similar to those of the HMOs and PPOs just described. The name of this plan says it all—the point, or place, where you receive the service affects your out-of-pocket cost. Under this plan you:
- May use specific doctors who are members of the network and pay the low co-pay (similar in cost to an HMO).
- May select from a list of doctors outside of the network, but who are affiliated with the plan, and pay a higher co-pay (similar in cost to a PPO).
- May select a doctor not affiliated with the plan at all and pay the highest co-pay and possibly a deductible (an amount you pay before your health care plan starts paying your health care claims).
Your doctor’s office usually submits your claims to the POS for you. The POS in turn sends you an EOB.
Indemnity Plan
This is a fee-for-service plan. You can go to any doctor you choose, including a specialist—no permission required. These plans, though, are often more expensive than plans described above. And, they typically only cover medical expenses related to illness and accident, not preventive care. Under this plan you:
- Pay an annual deductible.
- Pay a co-pay for doctor’s visits.
- Pay a portion of each medical expense. Often you’ll see an 80/20 split, which means your health care plan would pay 80 percent of the cost of your service; you’d pay the remaining 20 percent.
- May be required to pay for services up front and then submit the bill to your health care plan administrator for reimbursement.
Exclusive Provider Organization (EPO)
There are two types of EPOs. The first operates like an HMO, but EPO health care providers are not employees of the organization. An insurance company generally manages an EPO while an HMO is a business unto itself. The second type of EPO, which operates like a PPO, is used by employers. Each employer has a unique EPO. The name of the insurance company providing the benefits is displayed on health care plan documentation (not the name of the employer). An EPO may be insured or self-funded by an employer.
Next Section: Your Medical Coverage – What You Need to Know
